Perspectives on the Quality of Cancer Care in the U.S. and Latin America
Story By: Alexander Aviles
Two leading Latino oncologists discuss the promise of therapeutic inroads and the challenge of expanding access to Latin America.
THE FUTURE OF cancer presents a bit of a paradox. On one hand, experts foresee cancer diagnoses and fatalities increasing sharply in the coming decade, with as many as 12 million cancer deaths worldwide per year by 2030. At the same time, technological breakthroughs and immunotherapy treatments in development offer the hope of better prognoses and higher survival rates.
Few physicians understand the promise and peril of these double trend lines better than Arturo Loaiza-Bonilla, MD, MDEd, FACP, Vice Chair, Department of Medical Oncology at Cancer Treatment Centers of America® (CTCA), a comprehensive cancer care network of hospitals and Outpatient Care Centers in five U.S. cities—Atlanta, Chicago, Philadelphia, Phoenix and Tulsa.
“In the areas of immunotherapies and targeted therapies, innovation is taking place across the board,” says Dr. Bonilla. “We’re seeing the emergence of a new paradigm of treating patients by looking at their genomics and DNA biomarkers, not just their type of tumor. The bottom line is patients are living longer and living better. It’s an exciting time for the field.”
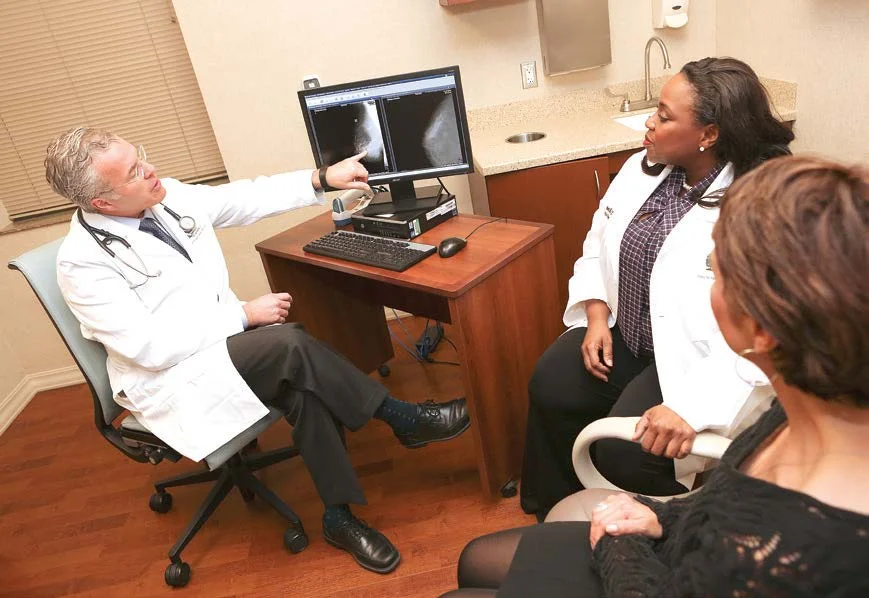
Consider breast cancer. The last few years have seen a revolution in the development and application of fresh combinations of new drugs (many of them less toxic) resulting in a significantly increased life expectancy for many patients. This is enabled by doctors’ growing ability to identify and precisely target multiple sub-groups of cancer in a way that would have been unimaginable a decade ago.
Sadly, and for many reasons, opportunities to benefit from genomic sequencing, immunotherapy and other technological advancements are not equitably and geographically distributed. The new science requires high levels of specialization supported by sophisticated diagnostic and treatment technologies. These are mostly concentrated in the U.S., Canada and a few large Latin American capitals, notably Mexico City.
“Generally speaking, there is a resource and access problem in Latin America when it comes to the detection and treatment of cancer,” says Ricardo Alvarez, MD, MSc, Medical Director of the Breast Cancer Center and Director of Research at CTCA®. “In many rural parts of Latin America, for example, it can be difficult to even find a physician who specializes in oncology. There are countries in Latin America where only one fellowship program exists in the entire country.”
This resource gap will come into even sharper focus in the coming years as the countries of Latin America undergo socio-demographic and epidemiologic shifts that produce higher rates of cancer for both men and women. Indeed, experts are stepping up warnings to the region’s health establishments to expand their traditional focus on infectious disease to include chronic
and lifestyle diseases like cancer as well.
Dr. Alvarez explains that the Latin American oncologists tasked with meeting the rising demand for specialized cancer care are often very well trained, but simply lack the resources to develop areas of expertise, or to contribute to the research and development of new treatments. Whereas treatment centers in the U.S. often contain divisions for each type of cancer, cancer care in Latin America remains much more one-dimensional, with corresponding cure rates.
“In much of Latin America, you do not find an environment favorable to innovation, and there are not the same opportunities for participating in clinical trials,” says Dr. Alvarez. “The situation won’t improve overnight; you can’t just train a million doctors and produce a research infrastructure at once. But it is getting better.”
Drs. Alvarez and Bonilla note that, in the meantime, experts in the region are pooling their knowledge in open-source collaborative projects that can make a big difference for their patients. They are also increasingly taking advantage of new communications technology to tap global expertise and maintain relationships with physicians in the U.S. and Canada. Through the emergence of telehealth, for example, physicians across hospital systems can work collaboratively and help provide treatment guidance to patients who lack the resources to travel.
“Virtual collaboration is very important in sharing knowledge across the western hemisphere,” says Bonilla. “By having organizations like CTCA communicate with physicians and colleagues in other countries, they help ensure that physicians have all the information they need regarding treatment options and clinical trials.”
U.S. physicians are helping to narrow the cancer care gap by developing “co-managed care” relationships in under-resourced regions of Latin America. For example, CTCA operates a “Mexico Physician Network” overseen by a surgical oncologist who maintains communication with leading doctors throughout Mexico. When their Mexican patients are candidates for treatments that are not available in, say, rural Durango, such as an immunotherapy or robotic surgery, an oncologist from the Mexico Physician Network can reach out to CTCA to explore different treatment scenarios, or possibly provide the patient with a second opinion.
“In Mexico City, or certain tier 1 cities, you find more mature infrastructure, academic networks and collaborations in place, but it's less available in other regions,” says Ananth Mohan, Vice President of New Ventures at CTCA. “So we contact specialized physicians that want to be part of an informal group that provides access to networks like CTCA, where they can benefit from knowledge-sharing and information on new therapies that are emerging in the States.”
Another way U.S. institutions can close the gap is through educational preceptorship programs that bring oncologists and surgeons from Latin America to U.S. hospitals for clinical seminars and mentoring. Sometimes these visiting physicians bring challenging case files and receive insights from conversations with host physicians and researchers.
“It’s a tremendous experience for physicians,” says Dr. Alvarez, who himself first visited the U.S. as a young doctor on a preceptorship from Argentina. “This is something that is very special to me. If you like to teach medicine or oncology, it provides a huge sense of satisfaction to help bridge the divide between North, Central and South America.”
And bridging geographic and socioeconomic divides is the key to improving cancer care, and health care in general, around the globe. The hope is for ever-improving outcomes in the future.